|
RACGP - Ulcer dressings and management. Geoff Sussman Background. Chronic leg ulcers caused by venous disease, arterial disease or a combination of both need to be clearly identified before treatment can be commenced. Their management will depend on the diagnosis, combining direct management of the ulcer as well as management of patient factors. 
Other chronic wounds commonly observed in practice include pressure wounds, skin tears, atypical leg ulcers. Objective/s. This paper will outline a simple way to manage people with chronic ulcers. Discussion. The prevalence of chronic ulcers in Australia has been estimated at 2–5%. Comprehensive assessment of the ulcer, the region and the whole person is an important first step in treatment. The aim of management is to promote healing and minimise the impact on the patient. Conclusion. The prevalence of chronic wounds is expected to rise given that people are living longer and that the incidence of diabetes is increasing. There is a need is to clearly identify the underlying cause of any wound, including factors that may delay healing, and to treat appropriately. Treatment should address the wound environment, tissue base, presence of bacteria and the level of slough. 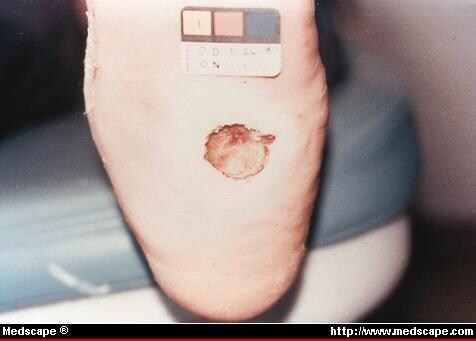
In patients with diabetes, any foot infection is potentially serious. Diabetic foot infections range in severity from superficial paronychia to deep infection. Find patient medical information for IODINE on WebMD including its uses, effectiveness, side effects and safety, interactions, user ratings and products that have it. BEST PRACTICE GUIDELINES: WOUND MANAGEMENT IN DIABETIC FOOT ULCERS 1 INTRODUCTION Introduction DFUs are complex, chronic wounds, which have a major long-term. Diabetic foot infections, which are infections of the soft tissue or bone below the malleoli, are a common clinical problem. Most infections occur in a site of skin. Original Article. Effects of an Angiotensin-Converting–Enzyme Inhibitor, Ramipril, on Cardiovascular Events in High-Risk Patients. The Heart Outcomes Prevention. 
If there is no improvement in wound healing after 4 weeks then seek help from a wound specialist. The most common chronic wounds seen in general practice are venous ulcers, arterial ulcers, mixed aetiology ulcers (venous and arterial), pressure ulcers, skin tears and atypical wounds such as vasculitic ulcers. Ulcer dressings and management . An estimated 400,000 Australians have venous leg ulcers (VLUs; Figure 1) due to chronic venous insufficiency (CVI). Original Article. Effect of a Multifactorial Intervention on Mortality in Type 2 Diabetes. Peter Gæde, M.D., D.M.Sc., Henrik Lund-Andersen, M.D., D.M.Sc., Hans. Diabetic foot problems eventually lead to lower limb amputations in some high risk persons. This article, written for physicians, summarizes the relevant data. Diabetes mellitus (DM) is a global epidemic, and diabetic foot ulcer (DFU) is one of its most serious and costly complications. DFUs result from a complex interaction. The management of ulcers is complex. Current practice varies in different clinical settings and treatments are often delivered by different healthcare professionals, who may or may not use best practice guidelines. 
The process described in this article is that used in the Therapeutic guidelines: Ulcer and wound management. The issue is not so much the choice of product but the accurate diagnosis of the underlying cause of the wound. It is often the case that a product is applied to a wound and when not successful the product is considered at fault so a different one is used; when that fails, the next product is used. The simple rule is to treat the whole patient and not the hole in the patient. The three principles of wound management are: Define the aetiology. Control factors affecting healing. Select appropriate local environmental management (dressings). Define aetiology. The most common chronic wounds seen in practice are: leg ulcers (venous, arterial, mixed)pressure woundsskin tears. Venous leg ulcers. An estimated 4. 00,0. Australians have venous leg ulcers (VLUs; Figure 1) due to chronic venous insufficiency (CVI). VLUs are managed in primary care or the community with variation in treatment and effectiveness,2 which in 2. The burden of recurrence is expected to rise with an ageing population and the growing epidemic of diabetes and obesity, which will further increase healthcare costs. VLUs result from the breakdown of the venous circulation in the leg and are associated with the inability of the leg to force the passage of blood through the various connecting veins via the bicuspid valves by muscular contraction. The increased venous pressure leads to pitting oedema, which in turn affects perfusion of the skin, so when some trauma occurs there is insufficient supply for healing to occur and an ulcer develops. Pitting oedema may result not only from chronic venous insufficiency but also organ failure, lymph disease or from medication (eg calcium channel blockers). Venous ulcers commonly develop in the lower one- third of the leg (the gaiter area) and are usually irregular in shape. Pitting oedema is usually present. The skin is often stained around the ulcer area because of haemosiderin deposition after leakage of red blood cells from the circulation. Typical features of venous ulcers include skin changes such as eczema or atrophy blanche (white stippled scars on the skin). The three most common risk factors for VLUs are a history of obesity, past deep vein thrombosis (DVT) and poor mobility resulting in venous stasis. In some cases, treatment includes surgery; however, the mainstay of treatment is the application of graduated compression therapy toe- to- knee (3. Hg at the ankle). It is, however, essential to exclude arterial involvement by testing the ankle brachial index or by ultrasonography. Lower limb exercise and addressing occupational factors, such as long periods of standing leading to venous stasis, should be encouraged. It is important to keep in mind that oedema may result not only from venous disease (pitting oedema), but also other causes including organ failure, lymph disease or from medication (eg calcium channel blockers). Lymphoedema is caused by a reduction in the function of the lymph vessels to drain extracellular fluid. The resultant oedema will place the patient at risk of ulcer development as a result of minor trauma and by the hyperkeratotic nature of the skin. Arterial ulcers. The death of skin automatically follows occlusion of its arterial blood supply unless this is gradual enough to allow a collateral blood supply to be established. Atheroma (thickening) is the most common cause of arterial ulcers of an ischaemic nature. Ischaemic pain, especially at night, is associated with arterial ulcers (Figure 2). This is as marked in small ulcers as in larger ulcers. Their edges are often sharply defined and the ulcer is . The base is often covered with slough. This may deepen to expose tendons. A history of intermittent claudication (pain on exercise), dependent foot (dusky foot) white on elevation, peripheral vascular disease, lower ankle brachial pressure index, weak/absent pulses, sluggish/poor capillary refilling may be present. Commonly, the ulcer site is below the ankles and on the foot or toes; however, arterial ulcers may be present on other areas of the body. The skin is often shiny and friable. Poorly controlled diabetes and smoking are significant risk factors causing arterial insufficiency. Treatment of arterial ulcers may involve surgical intervention for angioplasty, stenting, bypass grafting and, ultimately, amputation. Pain control is an important aspect of the management of arterial ulcers. Adequate analgesia is required to manage the severe ischaemic pain often experienced with arterial ulcers. These wounds should not have compression applied even if there is some associated venous disease. Venous/arterial or mixed ulcers. It is important to note that 1. These ulcers are often difficult to heal because of associated oedema, cellulitis, thrombophlebitis, rheumatoid diseases, particularly in patients who are bedridden, and malnourishment- related conditions of the skin in elderly patients. The most important issue is to determine whether the predominant cause is venous or arterial and then treat it. Graduated compression may be contraindicated, depending on the extent of the arterial component of the problem. If compression cannot be used it is difficult to address the venous component of the problem. Skin tears. Skin tears (Figure 3) are the most common wound type in the elderly population. If treated inappropriately, skin tears can become chronic wounds, exerting huge costs on the community and deleterious effects on the individual’s physical and psychological health. The ageing process will affect most of the structures of skin through loss of hair follicles, sebaceous glands that supply natural moisture to the skin, receptors, blood supply and sweat glands. The result of these tissue changes is that the skin becomes thinner and brittle, and the blood supply is reduced, fragile and more prone to injury. It is critical to identify patients at risk and then introduce prevention strategies. A recent study in Western Australia of 9. The management of a skin tear will depend on the level of damage. If it is possible to replace the flap, this should be done carefully, holding it in place with a few adhesive strips applied with no tension and covering with a silicone foam dressing, then covering with one or two layers of tubular compression bandages to apply mild pressure on the wound. This system is reviewed after 3 days then redressed every 5–7 days until the wound has healed. In addition to the more common forms of ulceration, there are a number of less common causes. Vasculitic ulcers may develop as a result of a number of medical conditions, such as rheumatoid arthritis and polyarthritis, which cause damage to the microarterial circulation by circulating antibodies. These wounds are often misdiagnosed as venous ulcers. If there is a dark wound margin, purple discolouration in the peri- skin and the wound is painful, suspect vasculitis. These wounds need to be treated systemically as well as topically. Pressure ulcers. Pressure ulcers (Figure 4) are the most preventable of all of the chronic wounds. Patients who are bedridden, for example, as a result of stroke, spinal injury, multiple sclerosis or dementia, often develop extensive pressure ulcers. These wounds may result from direct pressure, friction or shear injuries. A pressure wound develops when capillary blood flow to the skin and tissue over a bony prominence is decreased for a sufficient period of time. The consequence of the restricted blood supply is a reduction in oxygen supply and nutrition to the tissue, and inadequate excretion of the waste products. Friction. Friction occurs when the top layers of skin are worn away by continued rubbing against an external surface. This can be caused by ill- fitting footwear, or even bed linen, and can manifest in a simple blister or tissue oedema, or an open pressure wound. Shear. Shear occurs when the skin remains in place, usually unable to move against the surface it is in contact with, while the underlying bone and tissue are forced to move. This force will contribute to the destruction of microvasculature in a manner similar as direct pressure.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
